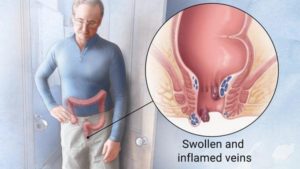
Hemorrhoids
Hemorrhoids are swollen and inflamed veins in the rectum and anus that are uncomfortable and can lead to itching and bleeding. According to Talley, “the prevailing belief is that chronic straining and the passage of hard stools results in a degeneration of the supportive tissue in the anal canal…leading to the development of hemorrhoids” (1). Furthermore, interventions that aim at reducing constipation are associated with relief and resolution of chronic hemorrhoids.
Illustration of hemorrhoids courtesy of the National Institutes of Health
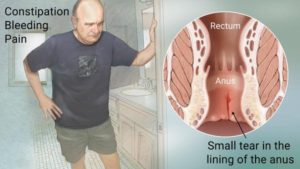
Anal Fissures
An anal fissure is a small tear in the anal tissue, brought on by the passage of hard stools. These tears can be further exacerbated by continued passing of hard stools. Increased dietary intake raw fruits, vegetables, and whole grains are associated with a decreased risk of anal fissures.
Fecal Incontinence
Stretching and weakening of the anal muscles and intestinal walls as a result of chronic constipation can lead to fecal incontinence, which is the accidental passing of solid or liquid stool from the anus. While constipation is not the only risk factor for development of fecal incontinence, it is nevertheless a risk factor. Fecal incontinence is the second most common cause for nursing home admissions. An embarrassing and debilitating condition, it occurs most frequently in the elderly.
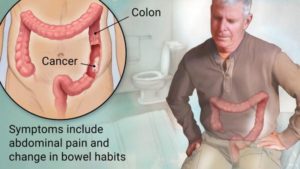
Colorectal Cancer
The causal ink between constipation and colorectal cancer has shown to be inconsistent in studies of colon cancer causes. Theoretically, longer transit time of stool passing through the colon leads to increased exposure of the colonic mucosa to carcinogenic substances in stool such as bile acids, fecapentaene-12, and ammonium acetate. Either way, doing all you can to facilitate the timely passage of stool through the colon is only of benefit.
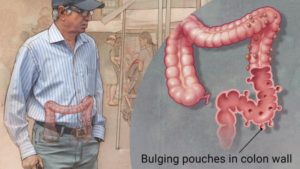
Diverticular Disease
Diverticular disease is the development of bulging pouches in the wall of the gastrointestinal tract. If these pouches become infected or inflamed, this painful condition is then referred to as diverticulitis. Diverticular disease is thought to be a result of a low fiber diet, which results in small, hard stools which changes bowel motility and puts an individual at risk for developing diverticula. Increasing dietary fiber intake with fruits, vegetables, legumes, and whole grains reduces the incidence and severity of this condition.
If you feel you are at risk for these conditions, visit your Physician or Nurse Practitioner and see if colon hydrotherapy might be beneficial in preventing these very uncomfortable and unhealthy conditions.